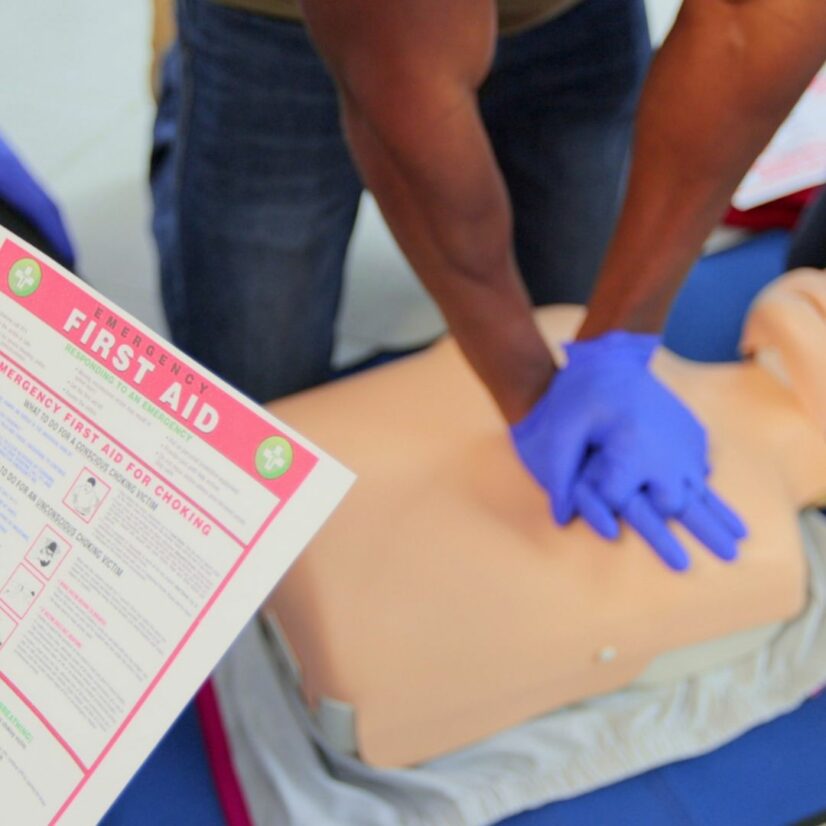
The Healthcare Foundation of New Jersey
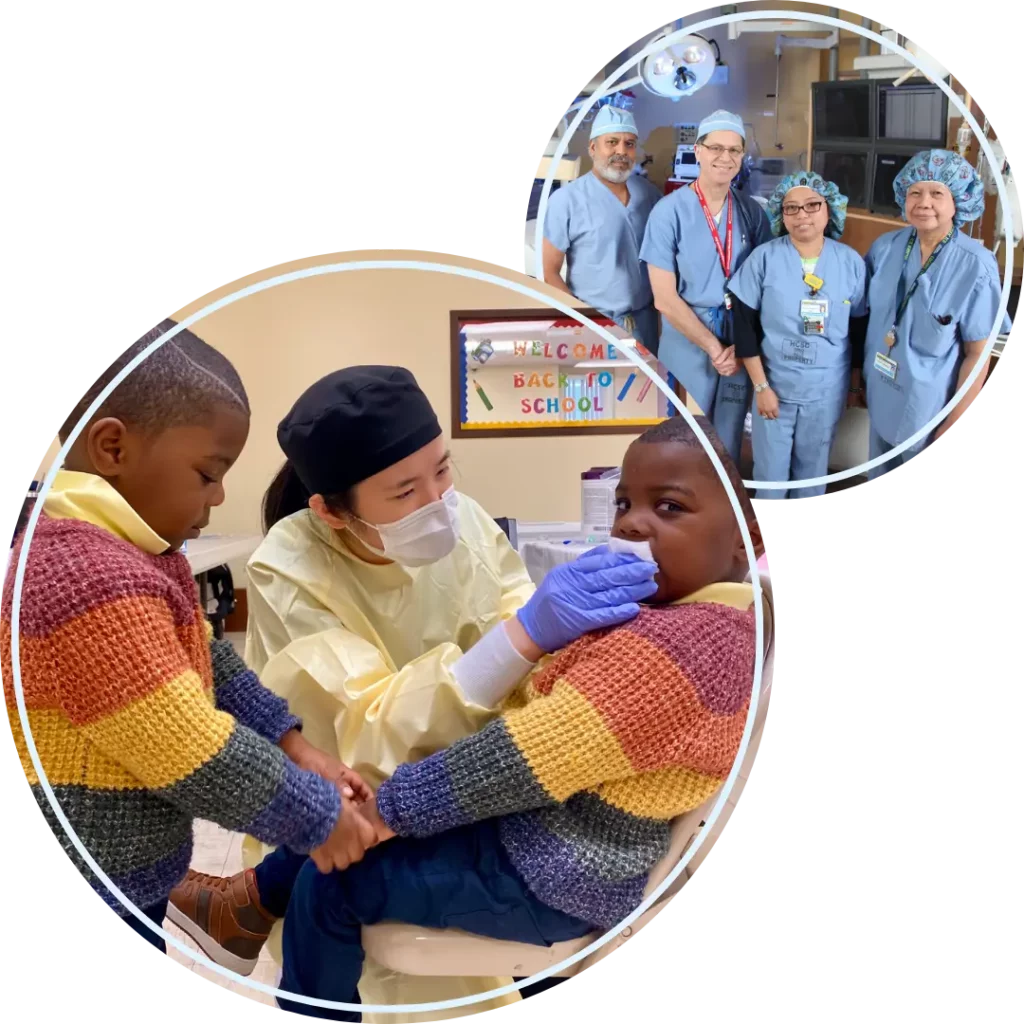
HFNJ is dedicated to reducing disparities in the delivery of healthcare and improving access to quality healthcare for vulnerable populations in Newark and its environs and the Jewish community of Greater MetroWest NJ.
$
1
Granted
1
Partners Funded
1